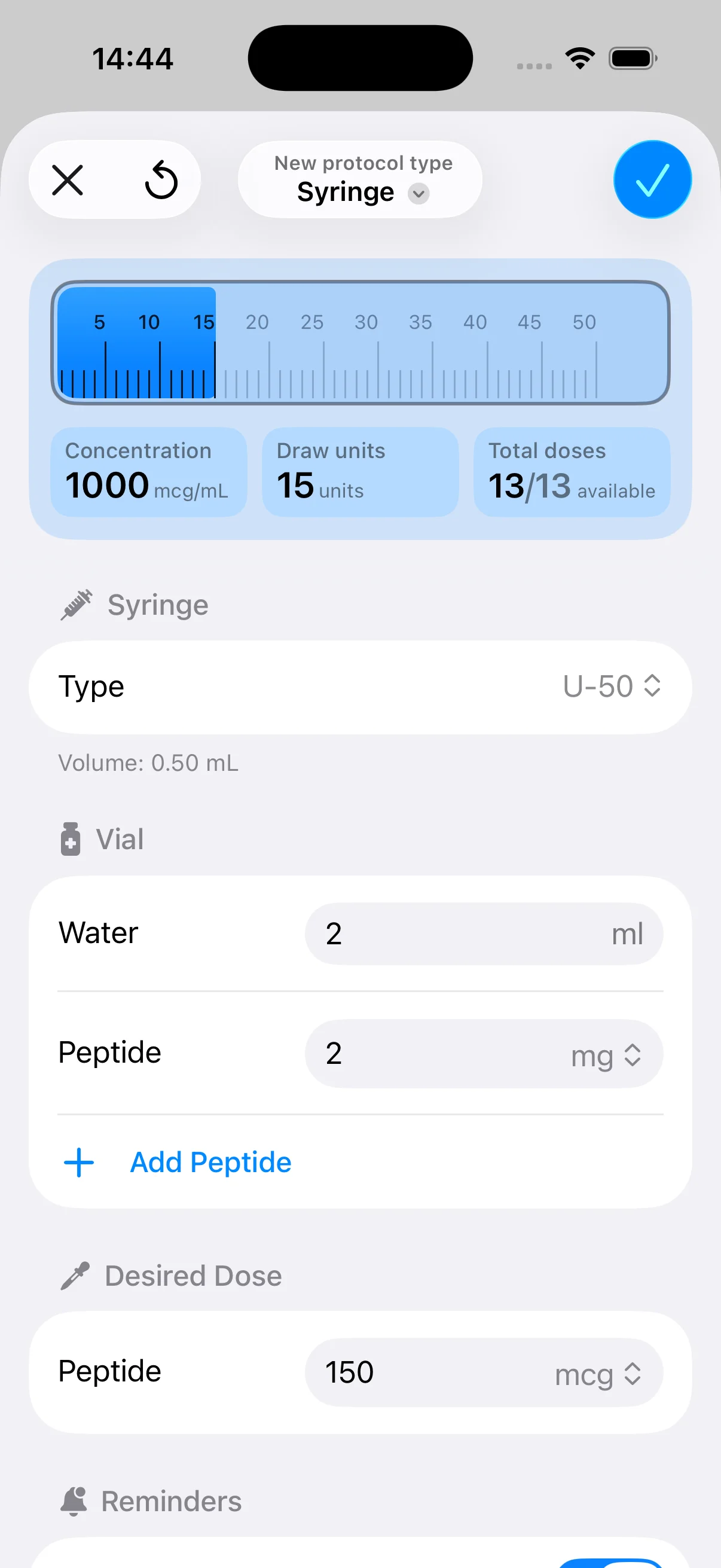
You’ve got a vial of peptide powder in one hand, a syringe on the table, and one immediate question in your head: what is bacteriostatic water used for, and do you need it?
If you’re running a home protocol, this is the point where people either get organized or make mistakes that ripple through the whole cycle. The peptide itself gets all the attention, but the diluent often decides whether your dosing stays accurate, whether the vial remains usable across repeated draws, and whether your routine becomes simple or messy. For most multi-dose peptide setups, bacteriostatic water is the practical workhorse.
It also isn’t some fringe product used only in obscure corners of the wellness world. The global Bacteriostatic Water for Injection market was valued at USD 1.22 billion in 2024 and is projected to reach USD 2.61 billion by 2034, with a CAGR of 7.9%, according to Market.us reporting on the BWFI market. That matters because it reflects broad use in pharmaceutical and hospital settings, not just gym-talk or forum lore.
For the home peptide user, the value is simple. You need a clean, repeatable way to turn a lyophilized powder into something you can dose accurately over time.
Table of Contents
Your Peptide Protocol Starts Here
The usual scenario is familiar. You open a package, pull out a small vial with white powder at the bottom, and realize the vial isn’t ready to inject. It still needs to be reconstituted, and the liquid you choose matters just as much as the math.

For home users, bacteriostatic water is usually the missing piece between “I bought the peptide” and “I can run this protocol safely.” It gives you a multi-dose diluent that’s built for repeated access, which is exactly how many peptide routines work in real life. You’re not drawing one large dose and tossing the vial. You’re often making a series of small, precise draws over days or weeks.
That’s why this topic comes up so often among people using compounds for wellness, fitness, body composition, or recovery support. The peptide may be the headline. The water determines whether your setup stays stable and manageable.
Why this matters for home users
Home protocols create a very specific problem. You need to:
-
Reconstitute accurately: the powder has to dissolve cleanly
-
Dose repeatedly: most users aren’t using the vial once
-
Avoid contamination: every puncture is another chance to introduce error
-
Keep the schedule clear: concentration and timing need to stay consistent
If you’re still doing hand calculations on scrap paper, a peptide calculator can make the concentration side much easier. That doesn’t replace proper handling, but it does remove one of the most common failure points.
Most peptide problems at home don’t start with the peptide. They start with sloppy mixing, unclear concentration, or repeated handling without a system.
Understanding Bacteriostatic Water’s Composition
Bacteriostatic water sounds technical, but the formula is straightforward. It’s sterile water with a small amount of preservative added so the vial can tolerate repeated use better than plain sterile water.

What is in the vial
Bacteriostatic water contains 0.9% (9 mg/mL) benzyl alcohol as a preservative and has a pH range of 4.5 to 7.0, with a nominal pH of 5.7, enabling safe multi-dose use for up to 28 days by inhibiting bacterial proliferation, as described by Sensorex’s overview of bacteriostatic water composition.
That phrase matters: inhibiting bacterial proliferation.
Bacteriostatic doesn’t mean it sterilizes a dirty process. It doesn’t mean it kills everything you introduce into the vial. It means the benzyl alcohol helps stop bacteria from multiplying the way they otherwise could after repeated punctures. That’s why it’s useful for multi-dose handling.
Why the preservative matters
Think of benzyl alcohol as a guard at the door, not a cleanup crew. If your technique is poor, it won’t rescue the vial. If your technique is clean, it gives you a margin that plain sterile water doesn’t.
That difference shows up in real home use:
| Feature | Bacteriostatic water | Why it matters |
|---|---|---|
| Preservative | 0.9% benzyl alcohol | Helps support multi-dose handling |
| pH profile | 4.5 to 7.0 | Supports compatibility and stability |
| Intended pattern | Repeated vial access | Better fit for peptide cycles |
| Role | Diluent, not active drug | Used to reconstitute other injectables |
A few practical points are worth keeping in mind:
-
It isn’t the medication: it’s the diluent that prepares the medication for use.
-
It isn’t a free pass for bad aseptic technique: alcohol swabs, clean handling, and proper storage still matter.
-
It exists for repeated access: that’s the core reason peptide users reach for it.
Practical rule: If your plan involves multiple pulls from the same reconstituted vial, you want a diluent designed for repeated use, not one intended for a single puncture and disposal.
The Primary Uses for Bacteriostatic Water
If you strip away the packaging and jargon, the main answer to what is bacteriostatic water used for is simple: it’s used to reconstitute injectable compounds that need to be drawn more than once.
Where it fits in a home protocol
The most common home use is drug reconstitution, which is identified as the primary use case for bacteriostatic water. Its 0.9% benzyl alcohol content enables multi-dose access for up to 28 days, reducing waste in protocols used for weight loss, performance enhancement, and biohacking, according to 360iResearch’s BWFI market analysis.
That maps directly onto how many peptide users operate.
You start with a lyophilized vial. You add a measured amount of bacteriostatic water. The powder dissolves into a solution. That solution then becomes something you can dose in repeatable, smaller amounts.
This is why it’s commonly used with compounds people discuss in peptide circles, such as HGH, HCG, BPC-157, and other multi-dose injectable preparations. The key advantage isn’t that bacteriostatic water is somehow “stronger.” It’s that it fits the workflow of repeated use.
Common use cases beyond peptides
The same practical logic explains its broader medical role. It’s used when a clinician or patient needs a sterile diluent for injectable medication that won’t be consumed all at once.
Common scenarios include:
-
Lyophilized powders: peptide and hormone products that arrive dry and need reconstitution
-
Subcutaneous dosing: small repeated injections where concentration control matters
-
Intramuscular preparation: when a product requires dilution before administration
-
General injectable prep: broader healthcare settings where repeated access to a vial is expected
What it does not do is replace protocol judgment. The right amount of water depends on the concentration you want, the syringe you’re using, and how easy you want each draw to be.
A concentration can be technically correct and still be inconvenient. Home users often make the mistake of mixing too little water into a vial, then finding that each dose is too tiny to measure comfortably. Others over-dilute and create bulky draws that make dosing clumsy. The best setup is one that is both accurate and easy to repeat without mental friction.
Bacteriostatic Water vs Sterile Water A Key Distinction
People often get tripped up here. Both products may look similar on a shelf. They are not interchangeable in the context of a multi-dose peptide routine.

The practical difference
The difference comes down to one thing: preservative content.
Bacteriostatic water contains benzyl alcohol, which helps inhibit bacterial growth in a multi-dose setting. Sterile water does not. That means sterile water is generally the single-use option. Once it has been used and exposed, the margin for repeated handling is gone.
For home peptide users, that changes the entire decision tree.
| Question | Bacteriostatic water | Sterile water |
|---|---|---|
| Repeated draws from same vial | Better fit | Poor fit |
| Multi-day protocol convenience | High | Low |
| Preservative present | Yes | No |
| Best use case | Multi-dose reconstitution | Single-use preparation |
Which one should you use
If you’re preparing a vial you plan to access again and again, bacteriostatic water is usually the practical choice. If a product specifically calls for another diluent, follow that instruction instead.
Use this quick framework:
-
One dose, immediate use: sterile water may be appropriate if the product calls for it.
-
Repeated use from the same vial: bacteriostatic water is the better fit.
-
Sensitive population or preservative concern: you need to assess compatibility first.
Using sterile water in a multi-dose home setup creates an avoidable contamination risk. The vial may still look fine. That doesn’t mean the handling choice was fine.
One more point matters. People often assume the liquid choice only affects sterility. It also affects routine quality. A protocol that requires repeated remixes, confusing disposal decisions, or unnecessary waste is harder to follow consistently. In home use, convenience and safety often travel together.
Proper Handling and Reconstitution Technique
The right diluent helps. Technique is what keeps the setup clean.

Multi-dose efficacy allows for 20 to 30 punctures per 30 mL vial over 28 days, and HCG reconstituted with bacteriostatic water maintains more than 95% bioactivity at 4°C for 28 days, according to DailyMed-linked product information summarized here. That tells you why proper handling is worth taking seriously. The product is designed for repeated use, but only if you treat it like a sterile workflow.
Before you mix anything
Start with setup, not speed.
-
Wash your hands: don’t skip this because you’re “only doing a quick draw.”
-
Clean the vial tops: swab both the peptide vial and the bacteriostatic water vial with alcohol.
-
Use a fresh sterile syringe and needle: don’t reuse gear for convenience.
-
Check the vial labels: confirm the peptide, the vial strength, and your intended mix volume before puncturing anything.
A lot of errors happen before the first drop enters the vial. Wrong vial, wrong volume, wrong assumption.
A clean reconstitution workflow
A simple workflow works best:
-
Draw the planned amount of bacteriostatic water into a sterile syringe.
-
Insert the needle into the peptide vial and let the liquid run down the inside wall of the vial rather than blasting straight onto the powder.
-
Allow the powder to dissolve gently. Swirl lightly if needed.
-
Don’t shake the vial. Rough agitation can be hard on delicate compounds.
-
Label the vial with the reconstitution date and your discard date.
That side-wall technique matters more than people think. It’s one of the easiest ways to keep reconstitution calm and controlled.
For a practical walkthrough on a common GLP-1 setup, this guide on how to reconstitute semaglutide is useful as a process reference.
Here’s a visual demonstration if you want to watch the handling flow:
Storage and discard rules
After mixing, your job isn’t done.
-
Store according to product guidance: many users refrigerate reconstituted peptides when appropriate for the compound.
-
Keep the stopper clean: wipe before each puncture.
-
Track the date: don’t rely on memory.
-
Respect the discard window: once opened, the multi-dose window isn’t indefinite.
The easiest way to ruin a good protocol is to turn the vial into a mystery. If you don’t know when you mixed it, how much you added, or how long it has been open, stop and reset.
Critical Safety Warnings and Contraindications
Bacteriostatic water is useful, but it isn’t universal.
Who should not use it
Bacteriostatic water is contraindicated in neonates because of benzyl alcohol’s risk of “gasping syndrome.” Some peptides, including certain GLP-1 analogs, may also show reduced efficacy or cause irritation when exposed to this preservative, as noted in Study.com’s summary of bacteriostatic water uses and warnings.
That means the default assumption of “bacteriostatic water is always best” is too simplistic.
If a patient is in a sensitive population, or if a compound is known to react poorly to benzyl alcohol, another diluent may be the safer choice. Home users should be especially careful here because online protocol discussions often flatten these distinctions.
When another diluent may make more sense
Use extra caution in these situations:
-
Neonates: bacteriostatic water is not appropriate.
-
Known benzyl alcohol sensitivity: avoid casual experimentation.
-
Peptide-specific compatibility concerns: check product guidance before mixing.
-
Irritation after reconstitution: don’t assume the peptide itself is the only cause.
A practical rule is simple. If the compound, manufacturer instructions, or prescribing guidance points to a preservative-free option, follow that instead of forcing a one-size-fits-all approach.
Frequently Asked Questions
Can you make bacteriostatic water at home
You can try, but you shouldn’t trust a DIY version for injection use. Home mixing doesn’t give you the confidence of properly manufactured sterile handling. For injection protocols, improvised shortcuts are the wrong place to get creative.
What happens if you keep using it past the discard window
You increase uncertainty. The problem isn’t just whether the vial “looks okay.” Sterility and stability become harder to trust after the recommended use window has passed. In a home protocol, once confidence drops, the vial should be discarded.
Do all peptides work well with it
No. Some do fine. Some may not. Compatibility depends on the compound and the formulation. If a peptide is known to be sensitive to benzyl alcohol, use the recommended diluent instead of assuming bacteriostatic water is automatically correct.
Can you inject bacteriostatic water by itself
It’s used as a diluent for injectable preparations, not as a standalone shortcut in a home peptide routine. Its role is to prepare another injectable compound for dosing.
What should you keep track of after mixing
At minimum, log:
-
The peptide name
-
How much water you added
-
The resulting concentration
-
The reconstitution date
-
The discard date
If you want a simple reference for common dosing and reconstitution terms, a peptide cheat sheet can help keep the basics organized.
PepFlow helps take the manual math and scheduling friction out of peptide routines. If you want a simple way to calculate doses, configure vial concentrations, track cycles, and stay on top of reminders without building your own spreadsheet system, take a look at PepFlow.