You have a new vial on the table, a syringe still in the wrapper, and a dose in mind. That moment is where most mistakes happen. Not because the process is complicated, but because small handling errors can turn a stable powder into an unreliable solution.
Freeze dried peptides are forgiving in one sense and fragile in another. They’re built to survive storage far better than liquid peptides, but once you open the vial and add diluent, precision matters. Clean technique, gentle mixing, correct math, and sane storage habits all determine whether the dose you planned is the dose you take.
Table of Contents
- Why Proper Handling of Freeze Dried Peptides Matters
- The Safe Way to Reconstitute Your Peptides
- Mastering Peptide Dosage Calculations
- How to Automate Dosing with the PepFlow App
- Storing Peptides for Longevity and Potency
- Avoiding Common Pitfalls and Troubleshooting Issues
Why Proper Handling of Freeze Dried Peptides Matters
Freeze drying exists because peptides don’t tolerate rough treatment well. Heat, moisture, and careless evaporation can damage delicate structures long before you ever touch the vial. In pharmaceutical manufacturing, that sensitivity is one reason lyophilization is used so widely.
Approximately one-fifth of the top 100 pharmaceuticals worldwide are freeze-dried, rising to almost half for biologics, according to OPTIMA’s overview of peptide lyophilization. That tells you something important. Freeze drying isn’t a niche trick. It’s a standard preservation method for molecules that lose reliability when handled the wrong way.
Why the powder matters
A freeze dried peptide arrives as a dry cake or powder because water has been removed through a controlled freezing and vacuum process. That dry state protects against the chemistry that makes liquid peptides less stable over time.
What you’re holding is the end product of a careful manufacturing sequence. The vial didn’t become stable by accident. Someone controlled freezing, drying, and packaging conditions so the peptide could stay usable until reconstitution.
Practical rule: Treat the reconstitution step like the final stage of manufacturing, not like casual prep.
That mindset changes how people handle the vial. They stop rushing. They stop shaking. They stop guessing at syringe units.
Precision is part of potency
Most users focus on dose size. Experienced handlers focus on the whole chain: vial condition, solvent choice, sterile technique, dissolution, calculation, labeling, and storage. A single weak link can make the dose less accurate even if the math looked right on paper.
The good news is that the protocol itself is straightforward when you stay disciplined:
- Keep the workspace simple: Clean surface, organized supplies, no distractions.
- Handle the vial gently: The peptide cake can be more fragile than it looks.
- Respect reconstitution: Once liquid is added, the storage logic changes.
- Document what you did: Date, solvent volume, concentration, and intended dose matter later.
Freeze dried peptides reward consistency. If you build a repeatable routine, you reduce contamination risk, avoid concentration errors, and make every later step easier.
The Safe Way to Reconstitute Your Peptides
The reconstitution step is where stable powder becomes a working solution. Done well, it preserves the integrity of the peptide. Done poorly, it introduces contamination, concentration errors, or physical stress that didn’t need to happen.

Why the powder is stable and the liquid is not
Freeze drying is gentle because these molecules often can’t tolerate aggressive conditions. In production, primary drying requires tight control around the product’s collapse temperature, often between -34°C and -25°C, because going above that can cause viscous flow and pore collapse, as described in American Pharmaceutical Review’s discussion of collapse temperature.
You don’t need to run a lyophilizer to benefit from that lesson. You just need to understand the implication. If the molecule needed that much care to become a stable cake, it makes no sense to blast it with rough handling once it gets to your desk.
A clean reconstitution routine
Set everything up before you start. Don’t open wrappers one-handed while holding the vial.
Use this prep list:
- Vial of freeze dried peptide: Inspect the cake before doing anything else.
- Sterile diluent: If you’re deciding between options, this overview of what bacteriostatic water is used for is a useful reference.
- New sterile syringe and needle: One for drawing diluent, separate injection supplies later.
- Alcohol pads: Clean both vial stoppers.
- Label or marker: Write the reconstitution date and final concentration immediately.
Then follow a fixed sequence:
- Wash your hands thoroughly.
- Clean the workspace.
- Wipe the top of the peptide vial and the diluent vial.
- Draw the exact volume of diluent you planned.
- Insert the needle and let the diluent run slowly down the inside wall of the peptide vial.
- Do not forcefully spray the stream onto the cake.
- Let the vial rest for a moment if needed.
- Gently swirl or roll. Don’t shake.
How to add diluent without damaging the vial contents
Most avoidable mistakes happen in the last three steps. Users jab the liquid straight into the cake, foam the vial, then shake because it didn’t dissolve fast enough.
That approach creates unnecessary stress. A slow stream against the glass is better. It wets the powder gradually and helps the cake dissolve more evenly.
If a peptide doesn’t dissolve instantly, patience is usually the right response. Agitation is usually the wrong one.
Some peptides dissolve quickly. Others need time. If the vial contains hydrophobic material or an uneven cake, dissolution can take longer. Gentle rotation beats aggressive mixing every time.
A short demonstration can help if you’re visual:
A few practical checks after reconstitution:
- Look for clarity: The solution should look uniform for that peptide.
- Check for stubborn particles: Give it more time before assuming failure.
- Label immediately: Concentration mistakes often begin with unlabeled vials.
- Refrigerate promptly if appropriate: Don’t leave the liquid vial sitting out while you do the math later.
Mastering Peptide Dosage Calculations
The math isn’t hard. The danger is that people do it while distracted, convert units in their head, then trust a syringe reading they never properly checked.
The cleanest approach is to separate the calculation into two steps. First find concentration. Then find the injection volume that matches your target dose.

The only formula you need
Use this logic every time:
- Convert the vial amount from mg to mcg.
- Divide total mcg by total mL added.
- That gives you mcg per mL.
- Divide your desired dose in mcg by the concentration in mcg per mL.
- That gives you mL to draw.
Written:
- Concentration = total peptide mcg ÷ total diluent mL
- Injection volume = desired dose mcg ÷ concentration mcg/mL
For quick planning, a dedicated peptide calculator is useful because it removes the usual unit-conversion mistakes.
Worked examples
Here are manual examples using common vial setups.
| Vial Size (mg) | Diluent Added (mL) | Concentration (mcg/mL) | Desired Dose (mcg) | Injection Volume (mL / Units on U-100 Syringe) |
|---|---|---|---|---|
| 5 mg | 2 mL | 2500 mcg/mL | 250 mcg | 0.1 mL / 10 units |
| 5 mg | 2 mL | 2500 mcg/mL | 500 mcg | 0.2 mL / 20 units |
| 10 mg | 4 mL | 2500 mcg/mL | 250 mcg | 0.1 mL / 10 units |
| 10 mg | 2 mL | 5000 mcg/mL | 500 mcg | 0.1 mL / 10 units |
| 2 mg | 2 mL | 1000 mcg/mL | 200 mcg | 0.2 mL / 20 units |
Notice what these examples teach. Different vial sizes can produce the same working concentration if you change the diluent volume accordingly. That’s why reading “5 mg vial” tells you almost nothing about your actual injection volume until you know how much liquid was added.
Where people slip
Most errors fall into familiar categories:
- Mixing up mg and mcg: This is the classic thousand-fold unit problem.
- Assuming syringe units are universal dose units: They aren’t. They only reflect volume.
- Forgetting the final added volume: If you planned 2 mL but added less or more, every later dose changes.
- Rounding carelessly: Tiny differences matter more when doses are small.
- Using memory instead of notes: The vial you mixed last week won’t stay perfectly in your head.
Dose logic: Syringe units don’t tell you what you’re taking. Concentration does.
If you’re coaching someone else or managing more than one protocol, write the final concentration directly on the vial or storage label. That’s the number that keeps the math anchored in reality.
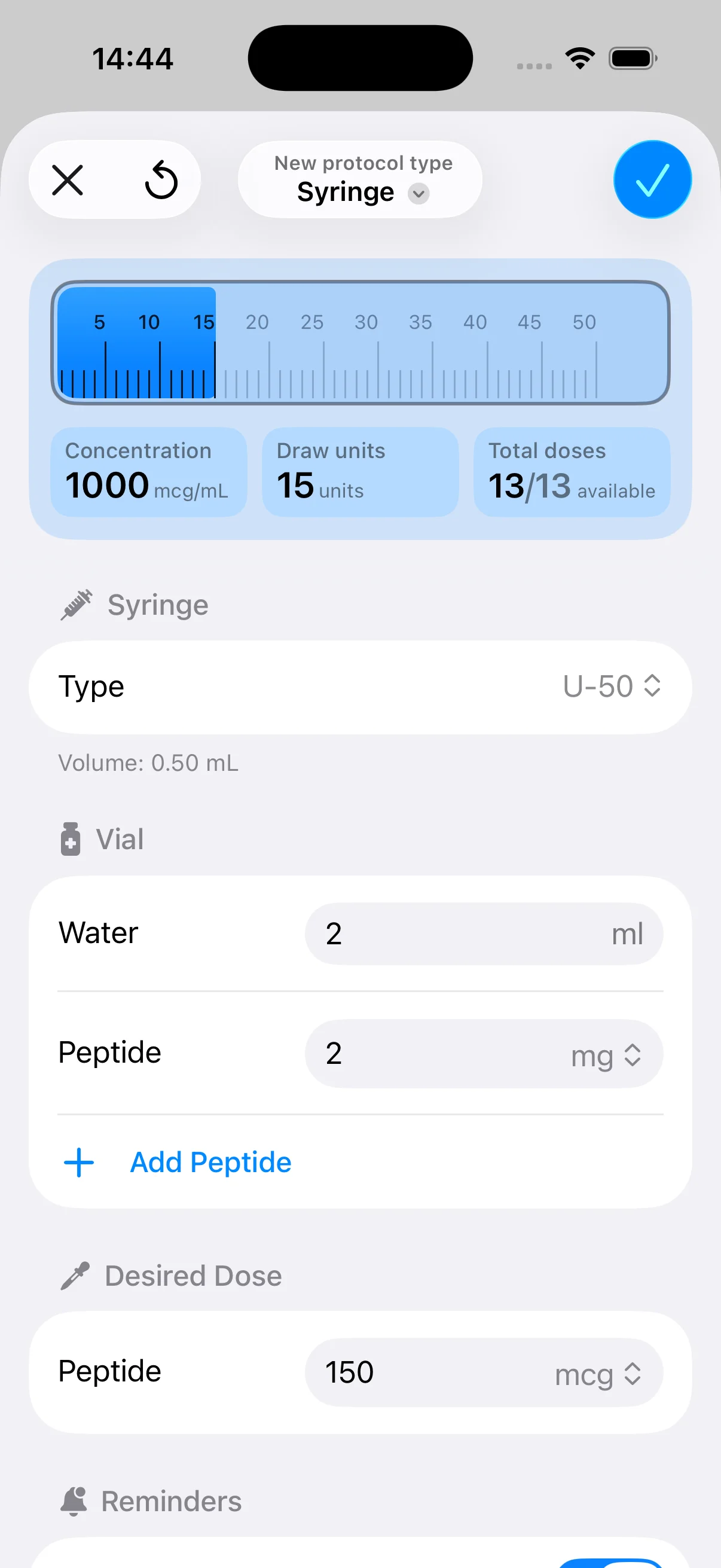
How to Automate Dosing with the PepFlow App
Manual math works when you’re fresh, focused, and dealing with one vial. It breaks down when you’re juggling different concentrations, changing schedules, travel days, or a stack of compounds that don’t share the same reconstitution volume.

Why manual math breaks down
People rarely make one dramatic mistake. They make a chain of small ones.
They remember the vial size but not the added volume. They know the target dose but forget whether that translated to 8 units or 10. They miss a day, shift the schedule, and then start estimating instead of following a plan.
That is exactly where a structured tool helps. PepFlow isn’t replacing judgment. It’s replacing the repetitive arithmetic and calendar friction that cause preventable errors.
A practical dosing tool should do three things well:
- Translate concentration into usable syringe volume
- Store the protocol so you don’t recalculate every dose
- Keep the schedule visible enough that skipped doses don’t turn into guesswork
A cleaner way to run a protocol
The strongest case for automation isn’t convenience. It’s consistency.
Once the vial is configured correctly, an app can hold onto the details you shouldn’t have to mentally reload each time. That includes concentration, dose target, timing, and reminders. If you’re running a cycle with pauses or specific frequencies, digital scheduling is safer than relying on a note app and memory.
This matters even more for users who adjust routines around training blocks, travel, or bodyweight-based protocols. The arithmetic may still be simple. The workflow usually isn’t.
A good digital routine also creates separation between planning and execution. You set up the vial once, confirm the result, and then follow the instruction rather than re-solving the same problem repeatedly.
The safest protocol is the one you can repeat without improvising.
That applies whether you’re running a basic single-peptide schedule or coordinating several compounds with different concentrations. The less often you recalculate by hand, the fewer opportunities you create for unit errors and skipped entries.
Storing Peptides for Longevity and Potency
Storage determines whether your peptide stays close to the condition it was in when you mixed or received it. Many users get the reconstitution step right, then slowly ruin the vial through sloppy storage habits.

How to store unopened vials
The key distinction is simple. Freeze-dried peptides in lyophilized powder form remain stable for several months to years when stored correctly, while reconstituted liquid forms are more vulnerable to hydrolysis and microbial growth, as explained in this overview of peptide stability after lyophilization.
That difference exists because dry powder has had water removed. Water is what allows many degradation pathways to become more active again.
For unopened vials:
- Keep them dry: Moisture is the enemy.
- Protect from light: A dark storage area is better than an exposed shelf.
- Avoid unnecessary temperature swings: Stability improves when the environment stays consistent.
- Open only when needed: Every extra handling event is another chance for condensation or contamination.
How to store reconstituted peptides
Once you add diluent, the strategy changes. Liquid peptides need colder, cleaner handling and more discipline.
Good habits include:
- Refrigerate promptly after mixing
- Keep the stopper clean before every access
- Limit repeated warming and handling
- Write the reconstitution date on the vial
If you draw from the same vial over time, contamination risk isn’t theoretical. Every puncture is an exposure event. The goal is to reduce how often the vial sits out, gets handled, or gets opened longer than needed.
Simple handling habits that protect potency
The best storage routine is boring. That’s a compliment.
Use a dedicated place in the fridge. Keep the vial upright. Store syringes and alcohol pads nearby so you aren’t hunting for supplies with the peptide warming in your hand.
A few extra habits help a lot:
- Date every vial: Don’t rely on memory.
- Record concentration clearly: Future-you shouldn’t have to reconstruct the math.
- Don’t keep “mystery vials”: If a label is incomplete, treat the vial as unreliable.
- Minimize access time: Take it out, draw accurately, return it.
Cold storage helps, but cold chaos doesn’t. A peptide stored at the right temperature and handled carelessly is still handled carelessly.
Avoiding Common Pitfalls and Troubleshooting Issues
Most peptide problems don’t begin with a catastrophic event. They begin with a vial that looked a little off, a solution that dissolved unevenly, or a handler who assumed “close enough” was good enough.
When the cake looks wrong
Not all freeze dried peptides arrive with the same cake structure. Some look uniform and solid. Others look airy, cracked, clumped, or partially collapsed. That matters because physical structure affects how evenly the peptide reconstitutes.
Improper freeze-drying without fillers can create fragile, uneven cakes that dissolve poorly and may lead to up to 20 to 30% variance in active peptide yield during reconstitution, according to Polaris Peptides’ discussion of cake quality and reconstitution variance.
That doesn’t mean every imperfect-looking vial is unusable. It does mean you should treat unusual cake appearance as a reason to slow down and observe carefully.
Use a basic visual check:
- Uniform cake: Usually the easiest to reconstitute predictably.
- Collapsed or sticky-looking material: May dissolve unevenly or cling to glass.
- Loose fragments on the vial wall: Add diluent slowly and let them wet before swirling.
- Unexpected discoloration: Treat with caution rather than forcing the process.
When the solution turns cloudy or slow to dissolve
Cloudiness doesn’t always mean contamination, but it does mean you should stop guessing.
Possible reasons include poor wetting, hydrophobic behavior, damaged cake structure, or incompatible handling. The fix is usually not shaking harder. The better response is to let the vial rest, then gently rotate it again.
If particles remain:
- Let the vial sit briefly after initial wetting.
- Roll or swirl gently.
- Check whether material is stuck above the liquid line.
- Avoid repeated violent mixing.
- If it still looks wrong, don’t assume potency is intact.
What not to do after a mistake
Some mistakes are recoverable. Some aren’t.
If you accidentally shook the vial once, don’t panic. Let it settle and inspect it. If you forgot to label it, correct that immediately while the details are still certain. If you no longer know how much diluent was added, stop there. An unknown concentration means every later dose becomes a guess.
The same rule applies to suspicious storage history. A peptide that was left warm, repeatedly handled, or exposed to moisture may still look fine while behaving unpredictably.
A peptide vial should earn your trust through clean handling and clear records. It shouldn’t get trust because you hope it’s probably fine.
That mindset prevents two expensive outcomes. Wasting product, and building a protocol around doses that were never accurate.
PepFlow helps remove the two failure points that cause the most trouble in peptide routines: manual dosing math and inconsistent scheduling. If you want a cleaner system for calculating syringe units, organizing concentrations, and staying on track with reminders, take a look at PepFlow. It’s a practical companion for people who want their protocol to stay precise from the first reconstitution to the last logged dose.